Step Zero.
I had an idea I posed to one of the nurses when I was in hospital: coma surgery. A patient comes in, they’re induced into a coma, and filed into a drawer (like they use in morgues) until their surgery. This would be perfect for people like me, who had to wait ten days. After the surgery, they’re stuck back in the drawer until they’ve healed. Then they’re awakened, and sent on their way.
I’m sure somebody unadventurous will point out the drawbacks of coma surgery, but I think it has a lot going for it. You don’t have to worry about hospital beds, about wasting hospital resources, and patients can sleep right through their experiences.
Not that that my experience was at all bad. In fact, my experience made everything tolerable.
The Paramedics
The paramedics arrived promptly, and I explained what had happened to me, and all my dietary intolerances and reactive hypoglycemia – just in case that had any bearing on my treatment. I then told them I was lucid now, but if I saw what was going on with my break (which was hidden under my tracksuit, sock, and runner) they’d lose me quick.
They gave me some sort of plastic canister to suck on which was meant to help nullify the pain, then got me into the ambulance. One of the paramedics held my leg in place while the other cut away the laces of my runner and my sock. At that point, I’m sure I felt my leg spread the way an egg would if you dropped it on the floor. Or maybe I’m just imagining it. The paramedics splinted my leg, gave me some morphine, checked my blood sugar, and brought me to the Austin, all the while assuring me, and warning me whenever the ambulance would hit bumps in the roads
Emergency
You hear a lot of horror tales about waiting in emergency rooms, although I don’t think you can blame hospitals for that. It just comes down to the amount of staff versus the amount of patients. (Possibly, another win for coma surgery!)
However, I was wheeled straight into an EMERGENCY room. I explained yet again what happened. I can’t recall if they gave me more drugs, although I’m sure they must’ve.
They removed the splint and fixed the dislocation in my ankle by lifting my leg by the foot until the foot socketed back into place. There was some pain, but it was more the discomfit associated with the knowledge of what was going on which was the problem. They then bandaged me (and maybe even plastered me – apologies on the details; not the best time to be recording every detail).
They also took my blood sugar again. As a reactive hypoglycemic, I’m meant to eat something every three hours, and I was now over that by half an hour, (not to mention the exercise of the walk usually depletes you also).
Then I shook for a bit, as shock set in.
Afterwards, I was wheeled into a bay, and taken for several x-rays. But it was a case of waiting until I was ready to be taken for surgery. I had to wait an appropriate amount of time since my last meal. (If you’re curious why, it’s because when you’re under anesthetic, any food in your stomach can regurgitate into your lungs).
Surgery
You get wheeled into surgery and are fully aware. But by the time they prep you, all you know is oblivion.
I did go in, though, thinking they’d fix my leg. That’s the plan when you come to hospital, isn’t it? I’m sure I might’ve talked to the surgeon about it while I was drug-induced and hazy, but can’t recall if I did.
I did think I’d wake up on the road to recovery.
Post-Surgery
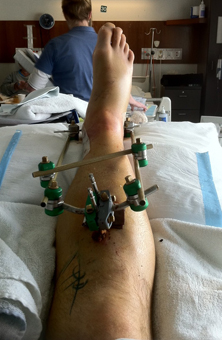 When I awoke and the doctors came around to examine me, I found they’d fitted an ‘external fixture’ to my leg – or an ‘x-fix’, as they called it. It was explained that there was too much swelling to operate, so they had to use this as a temporary measure to hold the bones in place until the swelling had diminished so they could perform surgery, (and insert plates).
When I awoke and the doctors came around to examine me, I found they’d fitted an ‘external fixture’ to my leg – or an ‘x-fix’, as they called it. It was explained that there was too much swelling to operate, so they had to use this as a temporary measure to hold the bones in place until the swelling had diminished so they could perform surgery, (and insert plates).
It was Friday. I was told they were aiming to perform the surgery on Sunday. Three days!
So began life in hospital. Nurses would come around and check me periodically, asking me to rate my pain out of ten, offer painkillers, take the pulse in my foot (which was very faint because of the swelling), and check my blood pressure, temperature, and oxygen levels.
I was very disoriented the first few days – possibly a combination of shock and an acclimation to all the painkillers. And I refused to look at the x-fix, keeping the sheet over it at all times, and telling the nurses when they came to examine me that I didn’t want to see it.
The most humbling thing was being confined to the same position in bed – on my back, with my foot propped up under a ton of pillows and usually packed in ice, (all in an effort to reduce swelling). This position became my world. I ate in it. I watched TV in it. I spoke on the phone in it. I washed in it. I moved my bowels in it.
Mentally, it’s wrong. For example, at home, you don’t eat lunch on the toilet. Well, I don’t. It really compounded the dislocation of my situation, how everything was gone, how incapacitated this break had made me, and how reliant I was on staff.
Sunday came, and the surgeon decreed the swelling was still too severe for surgery. He explained that if he operated with the swelling as bad as it was, it could cause further complications – that he might not be able to close, for instance. He also told me that the break had wishboned, and tented the nerve, which is why they’d called him in at 11.00pm on a Thursday night to operate, because if they’d waited until Friday morning the damage could’ve been irreparable.
He rescheduled surgery for Wednesday – providing the swelling had gone down – and I started to get more comfortable with my situation. Not that I enjoyed it. One day when I had the curtains drawn and just after I’d moved my bowels and washed – exhausted and drained from what it takes to perform these every day requirements in this position – I cried, thinking how unfair it was, and unable to see when things would improve. I wondered if the woman who’d hit me was at home drinking coffees and enjoying herself.
Come Wednesday, my foot was deemed still too swollen, and the surgeon told me they’d aim for Friday afternoon, that he was off but would come in to do the surgery. I knew there was nothing to be done about it, but it was frustrating to be in limbo. Once the surgery was performed, then healing could begin. That was Step 1. But that wasn’t where I was at. I was in a holding pattern. Step 0.
Thursday night, the surgeon came in with a group of other surgeons, and again my foot was still considered too swollen. Discussing it, they said 7–10 days was standard in cases like this, and ankles were especially troublesome. Also, to my embarrassment, I found out I’d been addressing the surgeon as ‘Simon’ when his name was ‘Shane’. His colleagues started stirring him, calling him ‘Simon’, whilst one of the other surgeons assured me, ‘You have to laugh.’
I wanted to, but it wasn’t easy.
Saturday, the doctors did the rounds and deemed the ankle still too swollen, which deflated me. I’d been here ten days, and now had to wait another three. However, the surgeon came in an hour later and judged the swelling good enough to go.
Time to heal. Maybe.